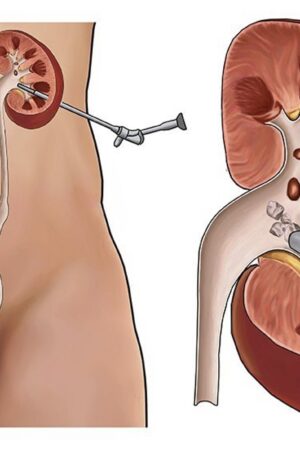
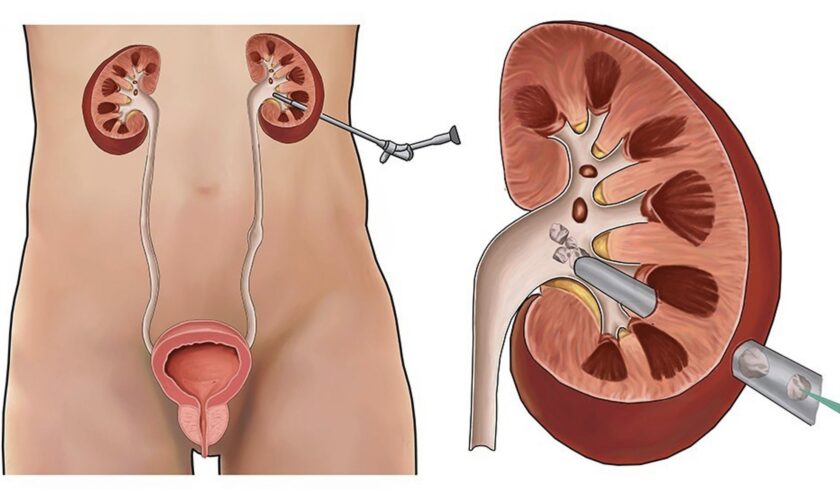
Percutaneous Nephrolithotomy, commonly known as PCNL, is a minimally invasive surgical procedure conducted to remove kidney stones. It is a safe and effective method that has been used for decades, offering relief from the painful symptoms of renal stones. The procedure involves making a small incision in the patient’s back and inserting a telescope-like instrument called a nephroscope to locate and remove kidney stones. PCNL is a complex procedure that requires skill and expertise from the surgeon, as it involves navigating through delicate tissues and structures of the urinary tract.
Say Goodbye to Kidney Stones
If you’re someone who has ever experienced the pain of kidney stones, you know just how unbearable it can be. However, there’s a solution that can help you say goodbye to kidney stones for good: percutaneous nephrolithotomy (PCNL). This procedure involves a small incision in your back to remove the stones directly from your kidney. While it may sound intimidating, PCNL is actually a highly effective and safe method for removing kidney stones. However, after the procedure, you may experience stent pain, which can be quite uncomfortable.
PCNL: The Stone-Crushing Superhero
If you’re suffering from a kidney stone, you know how excruciatingly painful it can be. But fear not, because PCNL is here to save the day! Dubbed the stone-crushing superhero, PCNL (Percutaneous Nephrolithotomy) is a minimally invasive procedure that can remove even the most stubborn of stones from your kidneys. And the best part? You can say goodbye to that awful stent pain. While stents are often placed to help with healing after the procedure, they can cause discomfort. Luckily, there are ways on how to relieve stent pain.
Breaking Down PCNL: How It Works
While Percutaneous Nephrolithotomy (PCNL) might seem like a daunting procedure to some, breaking it down into simpler terms can make it easier to understand. Essentially, PCNL is a minimally invasive surgical procedure used to remove kidney stones that cannot pass on their own. During the procedure, a small incision is made in the flank, and a scope is inserted to locate the stone. The stone is then broken up using a laser or ultrasound, and the fragments are removed through the scope.
PCNL may sound like a tongue-twister, but it’s a remarkable technique that has revolutionized the treatment of kidney stones. It’s a minimally invasive approach that maximizes results and minimizes risks. The procedure may seem daunting, but with the right team of medical professionals, it’s a walk in the park. So, if you or someone you know is struggling with kidney stones, fear not! PCNL is here to save the day (and your kidneys).